Primary left ventricular unloading in anterior STEMI without cardiogenic shock: Results from the STEMI-Door to Unload randomized clinical trial
Reported from ACC.26
Elad Asher provides his take on the STEMI-DTU trial, which was presented by Navin K. Kapur at the ACC.26 in New Orleans, and simultaneously published in the JACC.
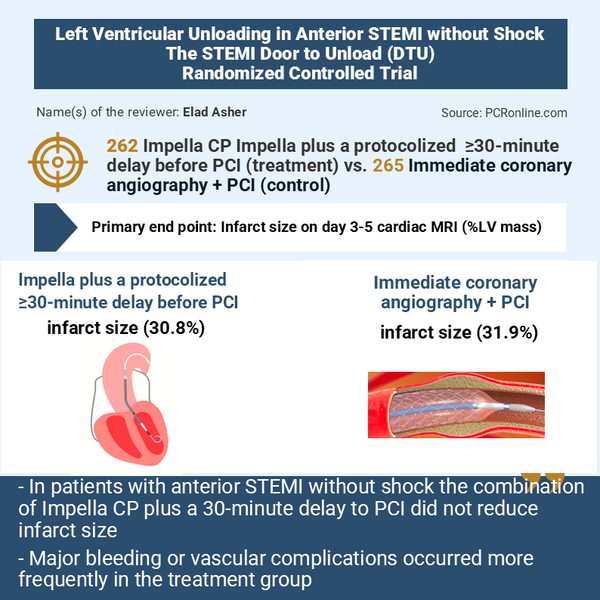
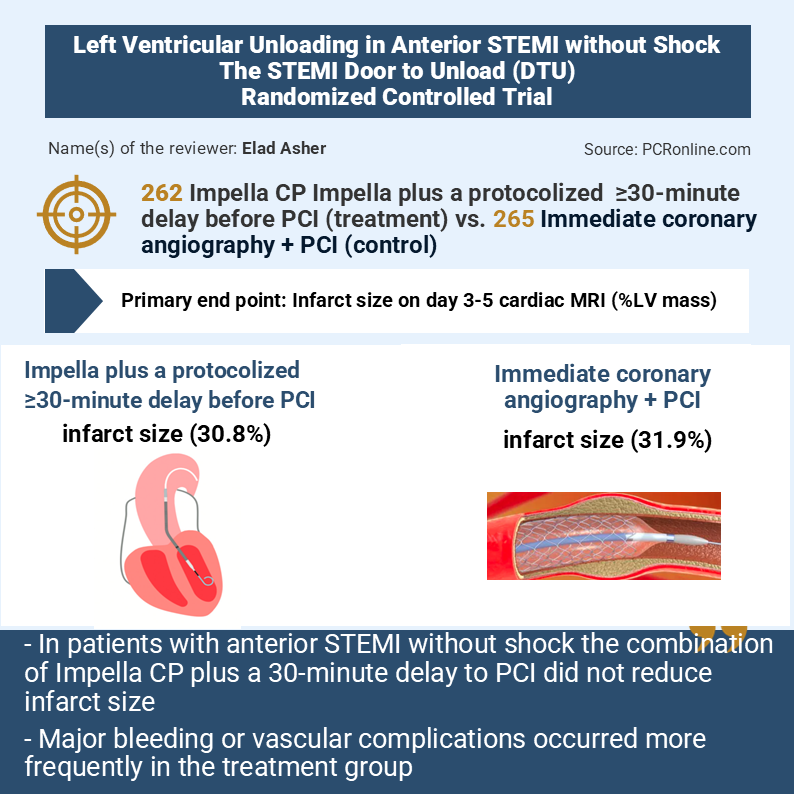
Designed by Elad Asher. Source: PCRonline.com
Why this study – the rationale/objective?
Acute ST-elevation myocardial infarction (STEMI), particularly anterior STEMI, remains associated with substantial morbidity and mortality despite timely reperfusion. Infarct size is a major determinant of outcomes, with even small increases translating into higher mortality and heart failure rates. Preclinical studies have suggested that left ventricular (LV) unloading prior to reperfusion may reduce myocardial injury by decreasing wall stress, improving coronary perfusion, and activating cardioprotective pathways.
Objective: To determine whether Impella-mediated LV unloading with a ≥30-minute delay before PCI reduces infarct size compared with immediate PCI in patients with anterior STEMI without cardiogenic shock.
How was it executed – the methodology?
A multicenter, randomized controlled trial conducted across multiple countries, enrolling patients with acute anterior STEMI.
Inclusion Criteria:
- Age 18–85 years
- First myocardial infarction
- Presentation within 1–6 hours of symptom onset
- Acute anterior STEMI with ECG and imaging confirmation
- Eligible for primary PCI
- No contraindication to Impella
Exclusion Criteria:
- Cardiogenic shock or mechanical complications
- Prior MI, CABG, or LAD PCI
- Inferior STEMI or RV infarction
- Prior fibrinolysis or mechanical circulatory support
- Significant aortic valve disease
- Cardiac arrest with neurological impairment
Study Design:
- Treatment arm: Impella CP insertion + ≥30-minute delay before PCI + 4–24 hours support
- Control arm: Immediate PCI
- Follow-up included cardiac MRI, echocardiography, and long-term clinical evaluation
Primary Endpoint:
- Infarct size (% of LV mass) on cardiac MRI at 3–5 days
Secondary Endpoints:
- Hierarchical composite including mortality, cardiogenic shock, heart failure, and device implantation.
- Safety endpoint: major bleeding or vascular complications at 30 days
Major findings
527 patients enrolled: 262 treatment, 265 control. Mean age ~61 years, ~79% male.
Baseline characteristics balanced, including hypertension (~40%), diabetes (~21%), and similar hemodynamics at presentation.
- No significant reduction in infarct size (30.8% vs 31.9%, p=0.50)
- All-cause mortality at 12 months was 4.0% in the treatment group vs 5.1% in the control group, and cardiovascular mortality was 3.6% vs 4.7%, respectively, with no statistically significant differences between groups.
- Longer ischemic time did not increase infarct size
- Major bleeding or vascular complications were significantly higher in the treatment group (34.0% vs 6.0%, p<0.001), primarily driven by access-site–related events.
- Possible signal of benefit in older patients (non-significant)
Critical reading and the relevance for clinical practice
This well-conducted randomised trial rigorously tested a novel physiological concept but failed to demonstrate clinical or mechanistic benefit. Despite strong preclinical rationale, LV unloading with delayed PCI did not reduce infarct size or improve outcomes, challenging translational assumptions. Importantly, delaying reperfusion under mechanical support appeared safe, which is clinically reassuring. However, the markedly increased bleeding and vascular complications—largely access-related—limit applicability. The study population (hemodynamically stable, hypertensive patients) may also have attenuated potential benefit. Overall, the findings reinforce the primacy of rapid reperfusion while suggesting that device-based unloading strategies require refinement before integration into routine STEMI care.
Should common practice and guidelines be changed?
Current evidence from the STEMI-DTU trial does not support a change in clinical practice or guideline recommendations. The strategy of LV unloading with Impella and delayed PCI failed to demonstrate a reduction in infarct size or improvement in clinical outcomes, while significantly increasing bleeding and vascular complications. Established guidelines emphasising rapid reperfusion with primary PCI remain strongly supported. Importantly, the findings suggest that delaying reperfusion, even under mechanical support, offers no clear benefit in this population. At present, this approach should be considered investigational. Future studies may identify subgroups or optimized protocols, but routine adoption into standard STEMI management is currently not justified.




No comments yet!