65 results
The future of aortic valve replacement - From index procedure to lifetime management
10 Apr 2026
A 68-year-old woman presents with symptomatic aortic stenosis and tricuspid valve anatomy, with no significant comorbidities and no evidence of coronary artery disease. Given her strong preference for a less invasive strategy, the Heart Team considers a transcatheter approach.
How would you treat this patient—and in case...

Author
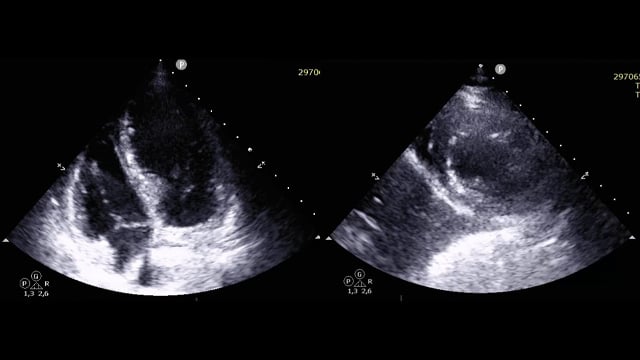
Transcatheter tricuspid valve replacement in carcinoid heart disease: A multimodality‑guided, patient-centered approach
03 Apr 2026
A 74-year-old woman with carcinoid syndrome develops progressive NYHA III dyspnoea and marked fatigue, despite well-controlled systemic symptoms. Echocardiography reveals torrential tricuspid regurgitation with carcinoid valve involvement, while surgical risk is deemed high due to age, frailty, and systemic disease. How would your Heart Team approach...

Author
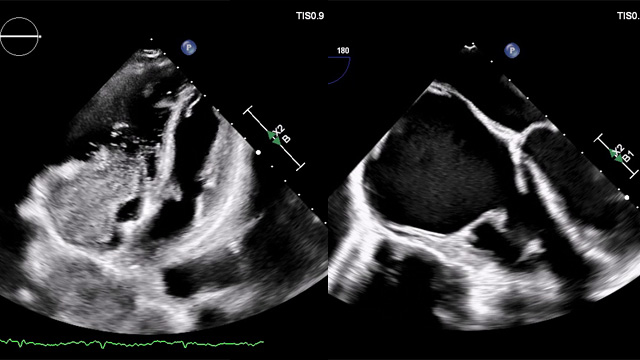
Mixed mitral valve disease in an irradiated chest with eggshell-like left atrium
27 Feb 2026
Managing mixed mitral valve disease is particularly challenging in patients with prior chest irradiation and extensive calcification.
A 40-year-old man presents with severe symptomatic MR, renal impairment, and an unusual eggshell-like left atrium. Imaging reveals complex mitral anatomy and critical constraints for transcatheter therapy.
How would you approach...

Author
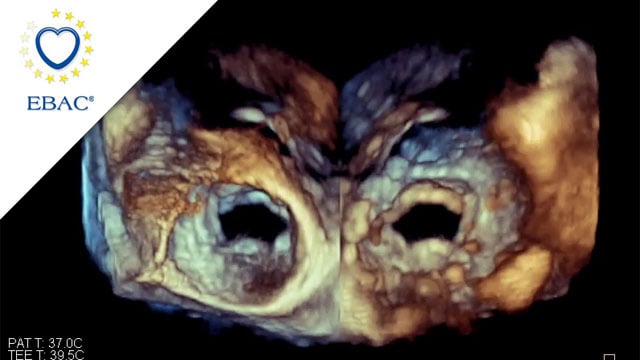
When a surgical valve needs a second life
27 Feb 2026
A 79-year-old patient previously treated with surgical aortic valve replacement was referred after an episode of acute cardiac decompensation. Although clinically stabilised, further evaluation revealed degeneration of the bioprosthesis, and mixed aortic valve pathology.
This case focuses on the diagnostic assessment and the strategic considerations guiding the...

Author

Interdisciplinary therapeutic strategy in a low-risk patient with aortic stenosis and preserved life expectancy
05 Mar 2026
A 71-year-old low-risk patient with symptomatic severe aortic stenosis and preserved ventricular function presents with progressive dyspnoea and chest pain. With long life expectancy, the choice of treatment demands careful interdisciplinary planning. How would you treat?

Author

Author

Author

Author

How should I treat a torrential tricuspid valve regurgitation in a young patient who remains symptomatic despite optimal medical therapy?
19 Feb 2026
A frail patient presents with worsening NYHA class III dyspnoea and peripheral oedema despite optimal medical therapy. Previously managed conservatively, severe tricuspid regurgitation has progressed to a torrential grade, with right-sided chamber dilatation and complex valve anatomy.
How would you treat this patient?

Author

Author

LAA closure with CT planning: challenging inferior chicken wing morphology
11 Feb 2026
This 77-year-old woman with paroxysmal AF and prior GI bleeding is referred for LAA closure, but CT reveals a shallow, inferior chicken-wing morphology that complicates device selection and planning. How would your Heart Team approach this challenging case?

Author

M-TEER with Mitraclip Gen5
03 Feb 2026
An 83-year-old female patient with HFrEF due to NICM and a history of arterial hypertension and persistent atrial fibrillation was referred with worsening exertional dyspnea, severe functional mitral regurgitation and moderate tricuspid regurgitation.
How would you treat this patient?

Author
A challenging valve-in-valve scenario in a patient with prior aortic coarctation repair
02 Feb 2026
This case features a 79-year-old patient with severe aortic stenosis and a degenerated surgical bioprosthesis, who previously underwent complex aortic surgery for coarctation.
Redo surgery was high-risk, so a transcatheter valve-in-valve procedure was chosen.
Explore the case to see how anatomy, prosthesis sizing, and vascular access options guide...

Author

Author

Author

Author

Author

Severe mitral regurgitation in a patient at high risk for surgery with a suboptimal anatomy for M-TEER: what other options can we find?
04 Feb 2026
A 78-year-old male presents with recurrent hospitalisations for HFpEF and severe degenerative MR. Multimodality imaging reveals fibro-calcific leaflet disease, restricted motion, and a short posterior leaflet, making him a suboptimal candidate for M-TEER and prompting consideration of transcatheter mitral valve replacement. How would you treat?

Author

Author
Author